Speak the Same Language as Your Consumer
Many hospitals tell us, “We know our community, but we don’t think they know us.” Too often, misinformation and misaligned campaigns create distance between hospitals and the people they serve. How can we close this gap so consumers feel heard–and health systems feel trusted? Both of these issues are often rooted in communication, specifically in the language both parties are using.
Language is more than the words that we use to communicate with one another. Language is a pillar of cultural identity. It shapes how people build common ground and express shared values. In healthcare, language is often where trust begins—or is broken. Yet despite its importance, the power of language is often underutilized.
When health systems learn to communicate and connect with patients in the language of their communities, they build more than understanding; they build belonging. Through proper language utilization, hospitals and health systems can position themselves as community members and contributors who help educate, connect, share, and humanize people’s relationship with healthcare.
Language is Lived Experience Turned into Words
Healthcare marketers often describe language as a vehicle for messaging. It’s how we communicate brand identity, convey expertise, or reassure patients in times of need. But for patients, language is not simply messaging; it’s lived experience turned into words.
When a patient says, “I just need someone to call me back,” they are not merely complaining about wait times; they are expressing a breakdown in trust and responsiveness. When another patient says, “My doctor really listened to me this time,” they are highlighting openness, empathy, and relationship, which are qualities that matter just as much as technical expertise.
As researchers who approach our work with an ethnographic lens, we don’t just document these words. We map them. We look for patterns in the terms and phrases (and sometimes even the body language) people use, and we plot those expressions on a map to show providers and marketers what patients are really saying about a particular topic. These language maps are more than academic exercises. They become strategic tools that help healthcare organizations align their priorities with the lived realities of their communities.
The Case of “Access to Care”
Let’s further examine a prominent topic in healthcare through the lens of patient language. Few words appear more often in healthcare than “access.” It shows up on websites, billboards, policy briefs, and strategic plans. But when you step into a patient’s world, “access” means something very different from what the industry typically describes.
Health systems define access through frameworks and structures—the five A’s, timely use of services, and barriers sorted by patient, provider, or system. Those definitions are accurate, but they rarely match how people talk about their actual experiences trying to get care.
When we explore the issues of access in open-ended qualitative interviews with patients, we uncover a much richer vocabulary. For example, patients don’t say, “I struggle with accessibility and accommodation.” They say things like:
- “I can’t get an appointment when I need one.” (Timeliness)
- “The clinic is too far from where I live.” (Proximity)
- “No one ever calls me back.” (Communication)
- “I don’t know who to talk to about my test results.” (Navigation)
- “It’s just too expensive.” (Affordability)
- “I wish my doctor would listen more before referring me out.” (Openness and willingness)
Patients don’t speak in institutional or policy terms. They speak in lived experience.
By breaking “access” into the words and phrases patients actually use, we see the nuance of how this issue plays out in real life. For patients, access is not just about locating a provider; it is the everyday experience of availability, responsiveness, affordability, and trust.
Language Mapping: A Strategic Tool for Holistic Planning
This method of language mapping identifies the clusters of terms patients use and the associations they have built between them. For example:
- Availability & Proximity: Patients link the presence of specialists, facilities, and diagnostics with whether they are “close enough” to use them.
- Timeliness & Urgency: Appointments, wait times, and time to diagnosis cluster together in patient stories.
- Openness & Relationship: Words around “listening,” “referring,” and “trust” emerge.
Hospital marketers and providers can use this information to close the gap between how they talk about an issue and how patients actually experience it. Mapping patient language provides a visual and strategic tool: a way to see not only what patients are saying, but how they are connecting concepts that organizations often address in silos. This is where healthcare marketers and strategists can step in.
While this article highlights access, the same principle applies to countless other healthcare issues. In each case, the words patients use to describe their needs reveal a reality that is often far richer and more nuanced than the frameworks professionals use to understand and address those needs.
For healthcare marketers and leaders, this is both a challenge and an opportunity. The challenge is to step outside of our own frameworks and lexicons. The opportunity is to listen, map, and integrate patient language into the very fabric of strategy and service design.
Language is a valuable tool for healthcare marketers to communicate their capabilities and intentions effectively with consumers. With the help of strategic aids such as language maps, marketers can close the gap between consumers and hospitals and find a common ground of mutual understanding that can be established and reinforced.
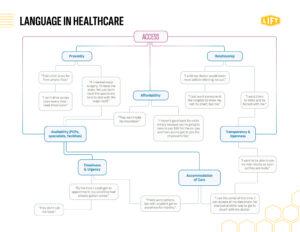
Build your common ground of communication with consumers by speaking THEIR language. Check out our example of a language map we’ve made about access using real patient data.

Kinsley Kilgore, MAPA, Ethnographer
Kinsley Kilgore helps hospitals, health systems, and public-health organizations see the human realities that shape healthcare decisions. At LIFT, she serves as both ethnographer and thematic analyst—conducting interviews, field studies, and qualitative syntheses that illuminate the emotional, cultural, and behavioral dynamics driving engagement across patient, caregiver, and community audiences.

Matthew Bradley, Healthcare Anthropologist
Matthew Bradley is a seasoned healthcare ethnographer with more than two decades of experience studying how people live, think, and make decisions about their health. Over the past 20 years, he has worked with pharmaceutical and life-science companies, hospitals and health systems, and clinical-trial research teams, contributing to initiatives that strengthen recruitment, retention, and real-world relevance.
